“Anorexia is the third most common chronic disease among young people, after asthma and Type 1 diabetes.”
~National Eating Disorder Association
Written by: Dr Kim Langdon MD
Reviewed by: Dr. RY Langham PhD
Table of Contents
Overview
Anorexia nervosa (AN), also known simply as anorexia, is an eating disorder that prevents a person from maintaining a normal or minimally-normal weight.
It is also an abnormal fear of weight gain, continuous attempts to control food intake, and a distorted perception of one’s own body weight and shape [3].
Types of Anorexia Nervosa
Anorexia nervosa is divided into two subtypes: restricting and bing-eating/purging.
The restricting type involves limiting food intake to the bare minimum to maintain a specific weight.
The binge-eating/purging type involves vomiting after ingesting food, using enemas, and/or taking laxatives or diuretics for weight management.
A recent study on eating disorders found that 0.2% of adolescents have anorexia nervosa, 0.6% have bulimia nervosa, 1.6% have a binge-eating disorder, 0.9% have a sub-threshold anorexia nervosa, and 1.1% have a sub-threshold binge-eating disorder [17].
A less recent chart from The National Institute of Mental Health shows the following lifetime prevalence of eating disorders for adolescents:
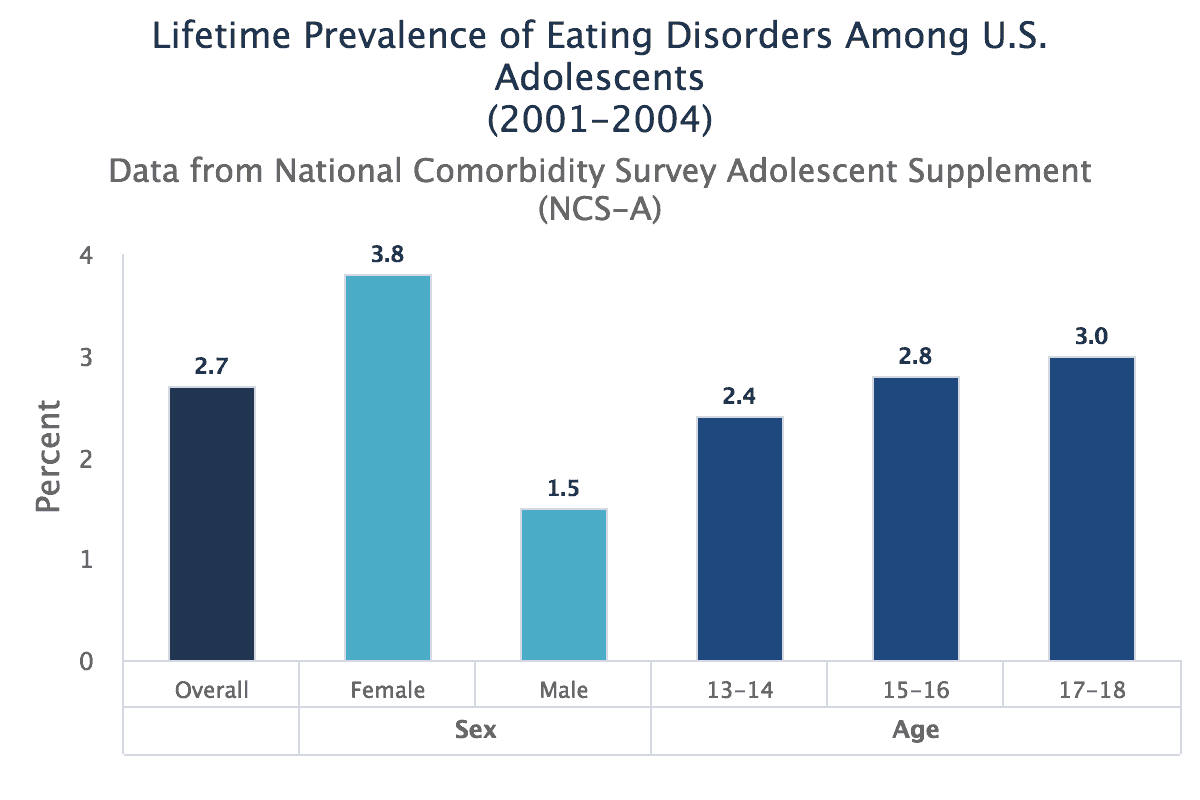
Symptoms
Common symptoms of anorexia include [8, 13, 14]:
- Temperature & Blood Pressure Fluctuations
- Sudden & Dramatic Weight Loss
- Dry, Flaky Skin
- Yellow Skin & Eyes (Jaundice)
- Baby-Fine Body Hair
- Blue Fingertips and Toes (Poor Circulation)
- Decreased Breast Volume
- Swollen Lymph Nodes and Jaw Glands
- Swollen Feet and Legs (Edema)
Causes
The exact cause of anorexia varies, but biological, psychological, and social factors appear to play significant roles in its development.
Still, in some cases, the cause is completely unknown.
Research suggests that if you have a history of depression and anxiety, you are more prone to developing anorexia than someone who does not have that specific background.
In addition, anorexia is more common in females than males, and adolescents develop it more often than older women.
Early-onset anorexia is linked to anxiety disorders. Ultimately therefore, anorexia stems from fear.
More specifically:
[thrive_custom_box title=”” style=”dark” type=”color” color=”#faf8d7″ border=”#000000″]
Anorexia is an attempt to control what happens to one’s body, because he/she is unable to control what is happening in his/her environment.
[/thrive_custom_box]
It is important to note, however, that contrary to popular belief, vanity (an obsession with being beautiful) is not linked to anorexia [18].
Risk Factors
There are several risk factors associated with anorexia, such as [18]:
- Break-ups
- Family Crises
- Divorce
- “Perfectionist” Tendencies
- Difficulty Communicating Negative Emotions
- Difficulty Resolving Conflicts
- Low Self-Esteem
- Inability to Face Age-Appropriate Challenges
- A Family History of Depression, Anxiety, and/or Eating Disorders
- Maternal Psychological Problems – i.e. Negative Expressed Emotions, Maternal Encouragement of Weight Loss, etc. [21].
Complications
Anorexia complications usually stem from starvation. Starvation leads to malnutrition, which leads to a protein deficiency and/or a disruption in multiple organ systems.
Listed below are common complications associated with this eating disorder [9, 11,12,13,14]:
- Delayed-Onset Puberty
- Lack of Menstrual Periods, Infertility, & Small Testicular Growth
- Low Estrogen Levels
- Underdeveloped Breasts
- Increased Growth Hormones
- Decreased Kidney/Adrenal Hormone Secretions
- Low Electrolytes – i.e. Potassium & Sodium
- Low Glucose Level – i.e. Blood Sugar
- Enlarged Heart – i.e. Rhythm Disturbances and/or Abnormal Heart Rate
- Low Blood Pressure
- Shock
- Kidney Malfunction – i.e. Kidney Stones, Swelling, and/or Elevated Levels of Waste Products (Nitrogen Build-Up)
- Dehydration
- High Cortisol Levels
- Stunted Growth
- Weak Bones
Prevention
The truth is, there is no way to prevent or predict this condition, but there is a way to treat it – if you know the signs and symptoms.
It is important to note that one study found that approximately 40% anorexia sufferers have at least one psychiatric condition, such as anxiety, depression, or ritualistic eating behaviors, and approximately 44% of them have family history of psychiatric disorders.
Therefore, it is important to pay attention to your child’s self-esteem and body image. More specifically, take note if your child experiences insomnia, uncontrollable crying spells, self-destructive tendencies, and/or suicidal ideation (suicidal thoughts) [19,20].
Here is a table from The National Institute of Mental Health that shows similar figures for how many sufferers of anorexia also have other psychiatric conditions:
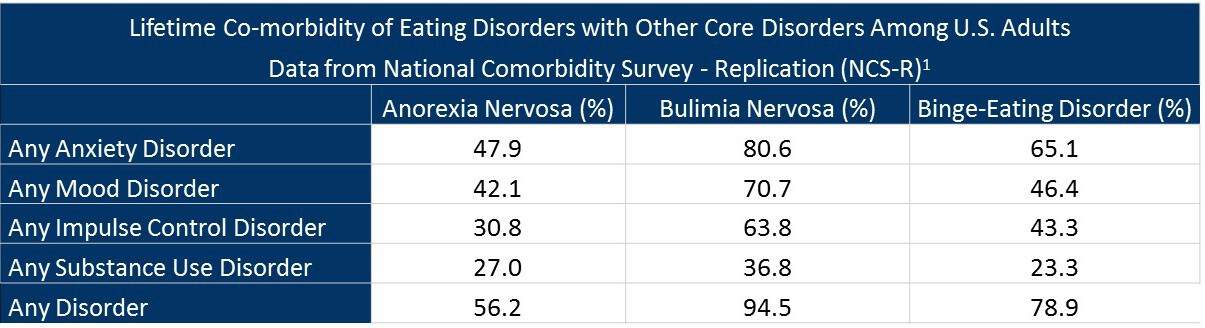
When to Seek Professional Help
It is important to recognize the early warning signs and risk factors (i.e. anxiety, depression, obsessive compulsive tendencies, etc.) associated with anorexia, so you can seek treatment for your child, as quickly as possible. Why? Well, because research suggests that early intervention and nutritional counseling can save lives.
Warning Signs
Early warning signs are [6,7]:

- A Dislike of Public Eating
- Continuous Complaints of Being “Fat”
- Repeatedly Looking into the Mirror
- Dressing in Loose-Fitting Clothes and/or Layering Extra Clothes to Disguise “Thinness”
- Frequent Bouts of Insomnia
- Social Isolation/Withdrawal
- Emotionless Expressions
So, if you notice that your child is playing with his/her food – i.e. moving it around on the plate, hiding some of it, and/or feeding it to the dog on a regular basis, you may have cause for concern.
Also, if your child’s clothes sizes never change – from year-to-year, you may want to consult a pediatrician to inquire about healthy growth curves.
It is important to understand, however, that anorexia treatment is multidisciplinary.
In other words, it includes: consultations with adolescent medicine specialists, nutrition classes, psychiatric or behavioral-developmental pediatrics, and/or psychotherapy sessions in some cases.
Therefore, if you notice any of the above symptoms or warning signs, seek emergency treatment.
Also, seek treatment, if your child expresses suicidal ideations (thoughts), psychosis, and/or “disordered” thinking [15,16].
Lastly, fainting, swollen extremities, and/or any other changes in appearance or behavior should be assessed by a healthcare professional [13].
Treatment & Therapy Options
If your child is diagnosed with anorexia nervosa, there are treatment strategies that can help.
These strategies include the following:
> Medical Management
Medical management involves correcting/preventing complications and re-establishing healthy eating patterns. If caught early and managed properly, hospitalization is rare.
> Hospital Admission
Hospital admission may be necessary for patients, who are extremely ill, and/or who have cardiac arrhythmia or severe metabolic abnormalities.
> Drug Therapy
Drug therapy is only required, when there is also a psychological condition like depression or anxiety. Prozac may beneficial for those suffering from depression, however, a common side-effect of the drug is sudden weight gain (in some people). Lastly, estrogen, commonly found in oral contraceptives, may be used to restore the menstrual cycles and preserve bone strength in females.
Current research suggests that drug therapy is most effective when combined with cognitive behavioral therapy (CBT). It is also recommended that one not take drug therapy alone. An low-dose of olanzapine, an anti-psychotic medication that alters your brain chemicals, may be useful for treating anorexia nervosa, especially if your child is hospitalized due to anxiety, obsessive eating practices, and/or failure-to-engage in the recovery process.
> Vitamins & Minerals Supplementation
Vitamins and minerals like vitamin D and calcium may help combat bone loss in anorexia sufferers.
Types of Psychological Therapy
Thankfully, there are also a wide-variety of psychological therapies that can help anorexics, such as [2,3,4,10]:
- Individual Therapy (Insight-Oriented)
- Cognitive Analytic Therapy(CAT)
- Cognitive Behavioral Therapy (CBT)
- Enhanced Cognitive-Behavioral Therapy (CBT-E)
- Cognitive Remediation Therapy (CRT)
- Interpersonal Therapy (IPT)
- Motivational Enhancement Therapy (MET)
- Dynamically-Informed Therapies (DIT)
- Group Therapy (GT)
- Family-Based Therapy (FBT)
- Specialist Supportive Clinical Management (SSCM)
- Conjoint Family Therapy (CFT)
- Separated Family Therapy (SFT)
- Multi-Family groups (MFG)
- Family Support Groups (FSG)
[thrive_custom_box title=”” style=”dark” type=”color” color=”#faf8d7″ border=”#000000″]
Note: The worst thing you can do is shame your anorexic child OR express negative emotions about his/her condition.
[/thrive_custom_box]
Also, don’t avoid or overly accommodate your child, because it may delay early treatment, which has been proven to help anorexia patients.
A nutritionist or dietitian should also be an integral part of your child’s treatment plan. And, while it is not known if a slow or aggressive food introduction is best for success, a comprehensive, individualized program is mandatory for recovery [5].
Outlook
Although anorexia cannot be predicted or prevented, early warning signs can signal a problem or a potential problem.
[thrive_custom_box title=”” style=”dark” type=”color” color=”#faf8d7″ border=”#000000″]
If your child experiences changes in his/her behavior, such as: avoiding school, an indifference to activities he/she used to enjoy, sudden weight loss, and/or altered food rituals, seek professional help as quickly as possible.
[/thrive_custom_box]
With quick action and therapy, this condition can be successfully treated, managed, and wrangled into control!
References:
1. Miller, K. K., Grinspoon, S. K., Ciampa, J., Hier, J., Herzog, D., & Klibanski, A. (2005). Medical findings in outpatients with anorexia nervosa. Arch Intern Med, 165(5), 561-566.
2. Eisler, I,, Simic, M., Russell, G. F., Dare, C. (2007). A randomized-controlled treatment trial of two forms of family therapy in adolescent anorexia nervosa: A five-year follow-up. J Child Psychology Psychiatry, 48(6), 552-60.
3. Morris, J., & Twaddle, S. (2007). Anorexia nervosa. BMJ, 334(7599), 894-898.
4. Waller, G. (2016). Recent advances in psychological therapies for eating disorders.
5. Katzman, D. K., Peebles, R., Sawyer, S.M., Lock, J., & Le Grange, D. (2013). The role of the pediatrician in family-based treatment for adolescent eating disorders: Opportunities and challenges. J Adolescent Health, 53(4), 433-40.
6. Kaplan, H., Sadock, B., Fleischer, G. R., Ludwig, S. (2011). Synopsis of Psychiatry.
7. Nicholls, D. E., Lynn, R., & Viner, R. M. Childhood eating disorders: British national surveillance study. Br J Psychiatry, 198(4), 295-301.
8. Price, C., Schmidt, M. A., Adam, E. J., & Lacey, H. (2008). Parotid gland enlargement in eating disorders: An insensitive sign? Eat Weight Disorder, 13(4), 79-83.
9. Sterling, W. M., Golden, N. H., Jacobson, M. S., Ornstein, R. M., & Hertz, S. M. (2009). Metabolic assessment of menstruating and non-menstruating normal weight adolescents. Int J Eat Disorder, 42(7), 658-663.
10. Wade, T. D., Frayne, A., Edwards, S. A., Robertson, T., & Gilchrist, P. (2009). Motivational change in an inpatient anorexia nervosa population and implications for treatment. Aust N Z J Psychiatry, 43(3), 235-43.
11. Ziora, K., Ziora, D., Oswiecimska, J., et al. (2008). Spirometric parameters in malnourished girls with anorexia nervosa. J Physiol Pharmacology, 59(6), 801-807.
12. Støving, R. K., Hangaard, J., Hansen-Nord, M., & Hagen, C. (1999). A review of endocrine changes in anorexia nervosa. J Psychiatry Res, 33(2),139-152.
13. Matzkin, V., Slobodianik, N., Pallaro, A., Bello, M., & Geissler, C. (2007). Risk factors for cardiovascular disease in patients with anorexia nervosa. Int J Psychiatry Nurse Res, 13(1),1531-45.
14. Vázquez, M., Olivares, J.L., Fleta, J., Lacambra, I., & González, M. (2003). Cardiac disorders in young women with anorexia nervosa. Rev Esp Cardiol, 56(7), 669-673.
15. Franko, D. L., Keel, P. K., Dorer, D. J., Blais, M. A., Delinsky, S..S., & Eddy, K. T. (2004). What predicts suicide attempts in women with eating disorders? Psychology Med, 34(5),843-853.
16. Holm-Denoma, J. M., Witte, T. K., Gordon, K. H., et al.(2007). Deaths by suicide among individuals with anorexia as arbiters between competing explanations of the anorexia-suicide link. J Affect Disorder, 107(1-3), 231-236.
17. Swanson, S. A., Crow, S. J., Le Grange, D., Swendsen, J., & Merikangas, K. R. (2011). Prevalence and correlates of eating disorders in adolescents: Results from the national comorbidity survey replication adolescent supplement. Arch Gen Psychiatry, 68(7), 714-23.
18. Macías-Robles, M. D., Perez-Clemente, A. M., Maciá-Bobes, C., Alvarez-Rueda, M. A., & Pozo-Nuevo, S. (2009). Prolonged QT interval in a man with anorexia nervosa. Int Arch Med, 2(1), 23.
19. Nilsson, E. W., Gillberg, C., & Råstam, M. (1998). Familial factors in anorexia nervosa: A community-based study. Compr Psychiatry, 39(6), 392-399.
20. Trace, S. E, Baker, J. H., Peñas-Lledó, E., & Bulik, C. M. (2013). The genetics of eating disorders. Annual Rev Clin Psychology, 9, 589-620.
21. Ammaniti, M., Lucarelli, L., Cimino, S., D’Olimpio, F. & Chatoor, I. (2010). Maternal psychopathology and child risk factors in infantile anorexia. Int J Eat Disorder, 43(3), 233-240.
22. National Eating Disorder Association. (2018). Eating disorder facts and statistics.








